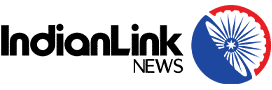Dr Haroon Qasim moved to Australia from India 20 years ago, seeking better working conditions and more opportunities for personal and professional growth.
“OECD countries offer better opportunities for research and development as well,” he tells Indian Link, unpacking the decision that saw him leave his country of birth.
Two decades on, this trend shows no sign of slowing down. The number of India-trained doctors moving to developed countries continues to grow, surpassing the number of professionals migrating from any other country.
AT A GLANCE
- A recent report has found that India-trained doctors practicing in OECD countries outnumber doctors trained in any other country
- Indian-origin doctors in Australia provide reasons for their own move away from the home country
- They offer suggestions on why – and how – India must strive to retain its doctors
According to a recent report by the Organisation for Economic Cooperation and Development (OECD), India has the highest number of doctors working in developed countries, with approximately 75,000 Indian doctors working abroad, primarily in English-speaking countries such as the US and the UK.

Pakistan comes in at number two, with more than 25,000 doctors working in developed countries, followed by Romania (21,800), Germany (18,827), and Britain (18,314). Russia, Egypt, and Poland are also included in the list. Although India has a severe shortage of doctors, compared to international standards, the number of doctors per thousand people in India is meagre. For example, the same OECD report shows that Austria has the best doctor-patient ratio in the world, with 5.5 doctors per thousand people, while India has only 0.9.

This brain drain of doctors is a significant problem for India, with Wollongong-based dentist Dr Ritesh Barua stating that “India has a shortage of doctors – more in rural areas due to disparity in the distribution of the doctors’ workforce.”
According to Melbourne-based Dr Raj Khillan, Victoria’s Australian of the Year, more than 5% of Australian doctors are trained overseas. The number of India-trained doctors though, is significantly higher. Still, he adds, “They form the major part of the medical workforce in the Western world.”
Renowned Sydney-based ophthalmologist Dr Sudarshan Sachdev AM, observes, “In the US, most Heads of Departments in leading medical institutions are India-trained doctors. Here in Australia too, many of our top specialists are from India. It’s a difficult decision to leave India, your support structure and especially your closest family, but Indian doctors have been leaving India for years.”
He himself moved to Australia way back in 1975, but claims he had never intended to do so.
“It was disheartening to find, upon graduating in the late 1960s, that there were no training positions open for me,” he tells Indian Link. “This despite the fact that I had finished with a gold medal.”
Ultimately he found one, but it was in the UK.
Returning to India seven years later, satisfactory employment continued to evade, while private practice was fraught with problems.
His doctor wife Naresh and he sought other opportunities overseas, and picked Australia.
The shortage of doctors in India is exacerbated by the fact that medical professionals are concentrated in metro areas rather than rural areas and villages, with more than 60% of India still living in the countryside.
Dr Barua believes that the lack of incentives from the government for doctors to move and stay in the country is a significant factor contributing to the brain drain.
Poor public hospital infrastructure, poor salaries, poor working conditions, and bureaucratic and political over-control of doctors are some of the reasons cited by Dr Raj Khillan.

Dr Khillan suggests that the Indian health system needs an overhaul, improving working conditions and upgrading facilities in the public system. “For example, doctors cannot be held responsible if there is a shortage of medicine for example. Doctors must be given control to manage hospitals and recruit eligible doctors, with less bureaucratic and political interference. Remove reservation systems in medical education and medical jobs to attract fairness in the system and get high-quality and meritorious doctors,” he says.
Dr Sachdev agrees.
“In my work to this day with Indian agencies, I see bureaucratic and administrative hassles, political considerations, even government interference.”
Patient culture is another issue, Dr Sachdev observes. “It is common to doctor-shop in India, for multiple opinions – but it can be frustrating to us as professionals.”
With general practice not as satisfying as it is here in Australia (because there seems to be less trust), and enough positions not available as specialists, the brain drain is but a natural progression.
Dr Barua believes better pay, respect, and working conditions would encourage doctors to stay on in the country.
“Now and then, one even reads reports about the doctor being bashed up by a relative of the patient. More protection and respect for the doctors would go a long way in preventing the brain drain,” he says.
“India should provide better incentives for young doctors to stay,” Dr Sachdev concludes. “They lack a clear pathway to professional development. And that’s a shame, as there’s no dearth of talent.”
READ ALSO: Dr Shailja Chanda OAM: “India must strive to retain its doctors”